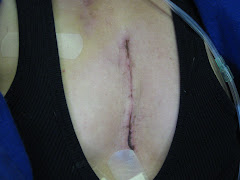
Open heart surgery was a major success! Jennifer's heart defects have been fully repaired.
The pulmonary vein anomaly, defined as a "congenital heart defect," existed since birth. The atrial septal defect, the hole between the right and left atrium chambers in Jennifer's heart, resulted from high pressures caused by the pulmonary hypertension.
The current belief is the pulmonary hypertension has been "neutralized." Meaning, what exists will remain but we're hopeful it will get no worse moving forward. We will learn more as we move along over the next few weeks.
The pulmonary vein anomaly, once thought to include only 1 of 3 veins on the right side of Jennifer's heart, was more extensive. All 3 veins needed to be "baffled" so oxygenated, "blue" blood could flow properly to the left side of the heart for distribution throughout the vascular system.
The surgeon, Dr. Ring, was prepared to address this additional complexity. Dr. Torres recommended Dr. Ring for this very purpose, knowing he would be poised and ready to handle complications in stride.
Improvements have been recorded for most of the vital pressure measurements, post-operation. Jennifer has achieved her goal, set so many months ago, of a successful surgical outcome.
Jennifer initially recovered in the ICU until Thursday night, at which point she was transferred around 10 pm CST to a "step down" unit in the Telemetry section of the hospital.
As of Friday morning, coinciding with the writing of this post, the plan and goal of medical staff is to discharge Jennifer later today or Saturday.
We are working through a few complications, which are not expected to persist. Jennifer is feeling nauseous, tired, and is in some pain, but all things considered we could not have scripted a better outcome.
There's a long road to recovery, which we can now focus on. The total rehabilitation period can last up to 3 months, with the first phase 6-8 weeks.
http://www.webmd.com/heart-disease/guide/heart-disease-recovering-after-heart-surgery gives some sense of what recovery will entail, as it talks about standard rehabilitation for overcoming heart surgery.
We have a new goal, which we're calling "back to basics." This means establishing a routine, to include things such as normal and deep breathing, eating a regularly, healthy diet, walking and other exercise, copious rest, etc.
This morning Jennifer had a bagel with cream cheese, banana, and cranberry juice. She's also taking 3 walks a day. In fact, Jennifer purportedly set a new speed record for walking the perimeter of the ICU. So we're on track.
A testament to the power of the human will, this experience has reinforced how blessed we feel to be surrounded by such a powerful support network.
Friends, family, colleagues and others have come to our aid, helping in any way possible to ease the burden Jennifer and her caregivers bear. When the load's been greatest, the support's been strongest.
The surgical team, physicians, nurses and others have all taken a special interest in Jennifer. It's clear her attitude and youth have won over their hearts, giving us a special level of care and oversight.
We hardly have a minute where someone's not coming by and checking on her health, making sure she's comfortable and disciplined about her recovery.
While some of you have heard this, it's worth repeating. Not all battles are won, and this war is far from over. But in the immortal words of Mark Twain "it's not the size of the dog in the fight, it's the size of the fight in the dog." Or in this case, the beautiful young woman.
 It has been more than 3-months since surgery and I feel great. A couple of scares since my last post, all of which occured in the Month of March.
It has been more than 3-months since surgery and I feel great. A couple of scares since my last post, all of which occured in the Month of March.