We were told to expect a 3-7 day stay in the hospital after surgery. Jennifer was in for 5. We’ve been in Dallas for a little over a week, since Sunday February 15th. The remainder of our stay in Dallas will be in a rental house we found on www.homeaway.com.
As with many caring for Jennifer, the anesthesiologist took a special interest, having felt an immediate connection. Young and female, she made sure extra care and attention was given to the suture.

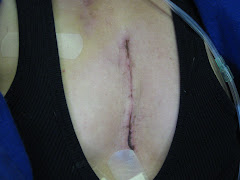
A comparatively small scar will result, ensured by the entire surgical team from incision to stitch. Jennifer’s scar will be a badge of honor, and serve to remind us of her strength throughout the process.
We are focused day-by-day on rehabilitation. Jennifer’s days are filled with rest, light eating, and a variety of light exercises. Nights are filled with intermittent sleep, early hour pain medication, and the occasional bloody nose.
Shortness of breath persists, even more so than before surgery. The culprit, at least partially, is atelectasis. A common postoperative complication, atelectasis is a collapse of lung tissue. It is a condition where the alveoli are deflated. Alveoli are "spherical outcroppings of the respiratory bronchioles and are the primary sites of gas exchange with the blood."
Jennifer’s oxygen saturation levels are below pre-surgery levels at rest and with exertion. More oxygen is required to maintain minimum desired level of saturation, 90%. What took 2-3 liters at elevation in Albuquerque is now taking 4-6 liters in Dallas.
At least for the near future, Jennifer is expected to maintain use of assisted oxygen and the intravenous medication Flolan. As we move along, levels of each will be lowered and Jennifer's reaction gauged. We are unsure what outcome can be achieved. While some Pulmonary Hypertension will always exist, we are hopeful we can eliminate the use of assisted oxygen and replace the use of Flolan with an oral medication.
Focusing on the present, Jennifer’s immediate goal is to complete breathing exercises every 2 hours, and to take increasingly longer walks every 4 hours. The respiratory exercises are done using an incentive spirometer. Anyone who’s suffered from a lung or heart ailment will remember this device, likely with disdain. But combined with very light physical exertion, its use is critically important. Walking consists of a few laps around the living room.
It is difficult to interpret what is attributable to surgical recovery and what our new “baseline” is. We continue to monitor Jennifer’s health closely, with pending follow-up appointments scheduled over the next week.
A good resource to plan for life after open heart surgery is named the AHA / ACC 2008 Guidelines of Adults with Congenital Heart Disease http://circ.ahajournals.org/cgi/reprint/CIRCULATIONAHA.108.190690.
As health care has advanced, a larger community of adults with congenital heart disease exists. Despite operative success, the condition should be monitored throughout life. With the importance often under-estimated, these guidelines are a great place to start.
Each day brings greater regularity. Small but important steps are being made towards realizing the benefits of surgery.





















5 comments:
thanks for all the updates! love the photos too :)
Hey, there! I'm glad to hear you're in a comfortable setting! The pics are great! You're in my thoughts constantly! I love you and look forward to your continued recovery! I MISS YOU!!! I'm around this week, as we are on winter break, if you'd like to chat! Sending lots of love!
Look forward to seeing you soon. This will be inspiration for a lifetime. Wishing you safe travels!
Jennifer,
I am so happy you are past your surgery and on your way to recovery. You are missed dearly her, know that we think and pray for you daily. Please let us know if you need anything, blessings always!
Lloyd
Hi Jenn. I'm glad the surgery went well! I pray that your recovery goes just as smoothly and the road back to health is not too difficult.
Love your cousin,
Marjorie
Post a Comment